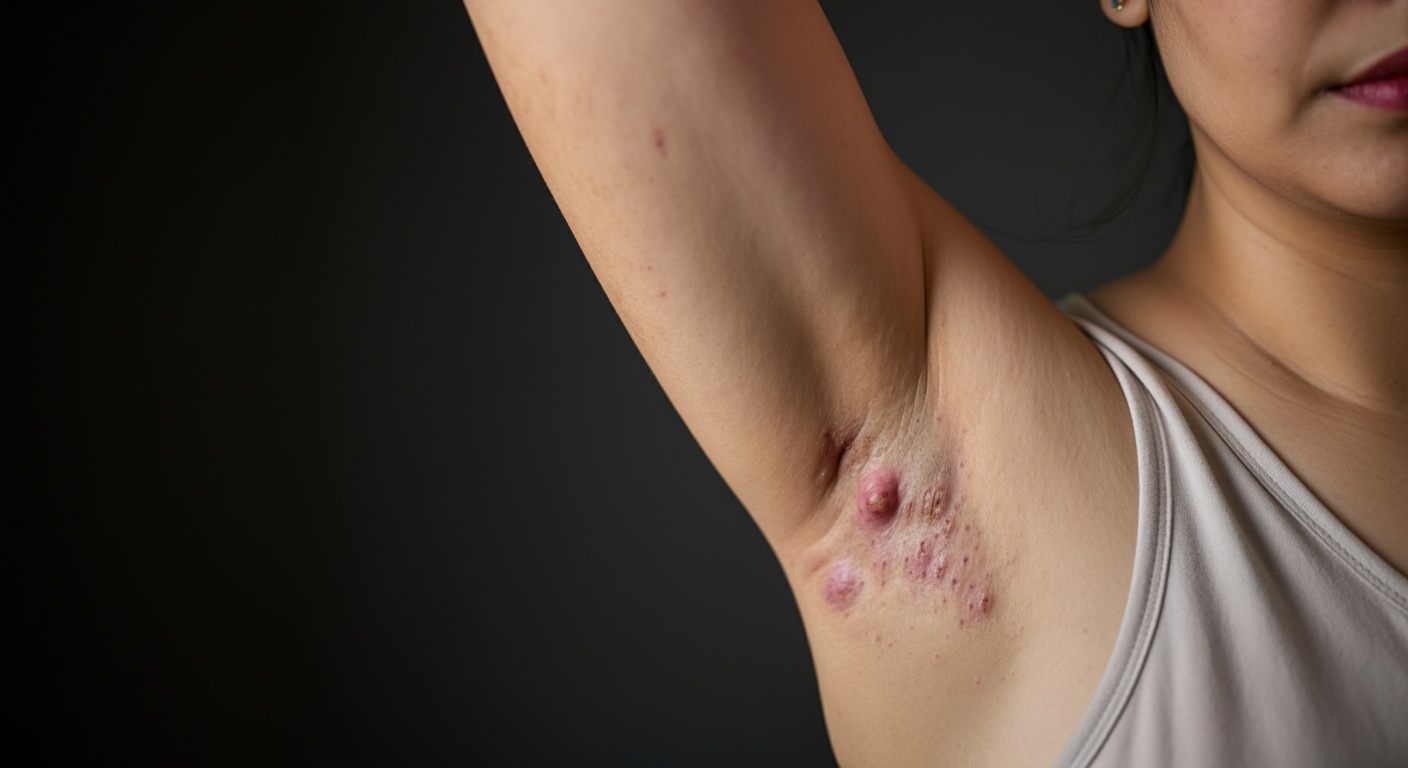
Hidradenitis suppurativa (HS for short) is a long-term and highly distressing inflammatory skin condition that causes painful lumps, oozing abscesses and scarring, often in areas like the armpits, groin, under the breasts and buttocks. Women in their 20s and 30s are more likely to be affected by HS than men and Black patients disproportionately suffer from the condition.
What is Hidradenitis suppurativa (HS) and how to recognise it?
“In the early stages, it can look like a recurring boil or ‘a spot that never quite heals,’” explains bodycare doctor, social media sensation and our October cover star Dr Kemi Fabusiwa, aka Dr Fab. “Over time, these lesions can link up under the skin, creating tunnels and thickened scars. It’s painful, unpredictable and massively under-discussed.”
“This complex and often misunderstood skin condition is characterised by painful, progressive inflammation of the hair follicles,” adds Nurse Teresa Tan, Aesthetic Medicine Award finalist 2025 and founder of skin clinic Tan&Co. “The underlying mechanisms of this ailment remain elusive. There is a common misconception that hidradenitis suppurativa arises from poor hygiene or is contagious, but this is not the case.
“It is believed that a blockage of the hair follicle by a keratin plug hinders the drainage of the associated glands. This blockage can trigger inflammation and rupture of the follicle, leading to the formation of abscesses.”
“Individuals with this condition may experience deep-seated nodules, draining sinus tracts, scarring, open tombstone comedones, and fistulas,” If left undiagnosed or untreated, these manifestations can significantly diminish a patient’s quality of life.”
HS is categorised into 3 ‘Hurling stages’ used to classify patients with HS into three disease severity groups:
-
Stage I – abscess formation (single or multiple), no sinus tracts or cicatrization/scarring.
-
Stage II – recurrent abscesses with sinus tracts and scarring, single or multiple separated lesions.
-
Stage III – diffuse or almost diffuse involvement, or multiple interconnected sinus tracts and abscesses across the entire area.
-
Patients experiencing stage III symptoms, the skin is often deteriorated in the affected areas, exuding large quantities of pus.
Individuals at higher risk for HS typically have a family history of the condition, obesity, type 2 diabetes, acne, or other inflammatory disorders. Smoking also increases the risk.
“The frequency and location of boils and abscesses can often indicate a higher likelihood of this condition,” continues Tan.
HS most commonly affects the armpit but also the groin, inner thighs, perianal areas, mammary and inframammary regions, buttocks, pubic region, scrotum, vulva, trunk, and, occasionally, the scalp.
“Early recognition of these symptoms is crucial for effective management and improved patient outcomes.”
Why is HS so often misdiagnosed?
Hidradenitis suppurativa is often misdiagnosed or underdiagnosed, particularly in its early stages, due to a lack of understanding and insufficient education regarding the condition. Plus, in early stages, HS doesn’t always look like HS.
“Early lesions can be mistaken for acne, folliculitis, or even shaving irritation. Add to that the fact that HS shows up in intimate areas and you’ve got a perfect storm of misdiagnosis and embarrassment,” says Dr Fabusiwa.
Clinicians need to start joining the dots earlier and ask about recurrence, location, pain, and drainage rather than treating every abscess as a one-off infection. Better education, earlier referral to dermatology, and more awareness of how it looks on different skin tones could completely change outcomes.
Why are Black women more commonly affected by HS?
Some data shows that Black women are disproportionately affected by HS experiencing higher rates of the condition and more severe symptoms. The reason remains unclear, but some research points to genetic factors.
Some research suggests potential differences in the anatomy of hair follicles or skin structure, but more studies are needed in this area.
“There’s definitely a biological piece,” says Dr Fabusiwa. “Genetics, hormones, and immune response play a part, but we can’t ignore systemic bias and access. Black women are less likely to be referred to specialists early, less likely to be believed about pain, and less likely to see clinicians who recognise HS on darker skin.”
Tan agrees that the problem is worsened for Black women thanks to institutional biases in the medical field.
“Black women are too often disproportionately overlooked or not taken seriously within healthcare settings. Long-standing medical myths and implicit biases can discourage Black women from seeking care, or result in their concerns not being fully heard when they do. In addition, much of the existing dermatological education and literature is centred on lighter skin tones, which makes conditions like HS more difficult to recognise on darker or melanated skin.”
“Dermatology needs to invest in inclusive research, visual education, and more diverse clinical trials,” adds Dr Fabusiwa. “We can’t solve a problem we’re still barely studying in the people most affected by it.”
The role aesthetic practitioners can play in HS support
Practitioners in aesthetic medicine are often the first point of contact for individuals seeking help for skin concerns, making them uniquely positioned to identify signs of HS early.
“Our role involves recognising when symptoms fall outside the aesthetic scope and may indicate a chronic medical condition,” says Tan. “By maintaining an informed awareness of how HS presents across different skin tones and body types, practitioners can help prevent delays in diagnosis.”
“When HS is suspected, practitioners should provide compassionate, non-judgmental support and guide patients toward the appropriate medical pathways, typically dermatology, primary care, or specialised HS clinics. Clear communication, reassurance, and sensitive handling are essential, as HS can be painful and emotionally distressing for patients.”
“That moment of empathy can genuinely change someone’s journey,” adds Dr Fabusiwa.
How is HS treated?
HS should be treated on a case by case basis depending on disease severity and hurley stage.
Treatment typically involves a combination of medical therapy, wound care, and when necessary, procedural or surgical intervention,” says Tan. “Current approaches described in dermatology guidelines and resources such as the BMJ, PCDS and BDNG emphasise early recognition, multidisciplinary care, and long-term management.”
Wound care is an essential part of HS treatment at all stages and may include:
• Regular wound assessment to evaluate inflammation, drainage, and healing.
• Appropriate dressings, such as silicone or silver-based dressings, to reduce friction, absorb exudate, and support healing.
• Specialised garments, such as HidraWear, which use perforated, low-friction materials to secure dressings comfortably.
Wound care helps reduce discomfort, minimise infection risk, and maintain quality of life.
Medical treatment aims to reduce inflammation, prevent new lesions, and manage flares.
• Topical antibiotics (such as clindamycin) can be used in milder disease to reduce bacterial load and inflammation.
• Oral antibiotics, like doxycyline, including tetracycline-class agents, may be prescribed for more persistent or widespread disease because of their anti-inflammatory effects. Retinoids are occasionally used too.
More severe HS may require escalation to systemic or biologic therapy:
• Biologic agents, such as adalimumab, are approved for moderate to severe HS and target the underlying inflammatory pathways.
• Surgery may be considered to remove chronically affected tissue, particularly when sinus tracts and scarring are extensive.
Aesthetic devices that can help manage HS:
• Carbon dioxide (CO₂) laser excision can be used to remove affected tissue with precision.
• Long-pulsed Nd:YAG laser may help by reducing inflammation and providing permanent hair reduction, which can reduce follicular occlusion.
• Photodynamic therapy (PDT) has also been used as an adjunct treatment in selected cases.
These options are often used for patients with recurrent lesions in localised areas.
How to advise patients to manage their HS
To help manage HS at home, Dr Fabusiwa advises patients to think gentle, consistent, and anti-inflammatory…
“Antibacterial washes like hibiscrub or benzoyl peroxide are important in the management of HS,” says Dr Fabusiwa. Patients should also avoid tight clothing or anything that increases friction.
“Warm compresses may provide comfort by soothing pain and supporting drainage during flares,” adds Tan. “Topical ingredients like zinc and niacinamide can help calm inflammation and strengthen the skin barrier, while resorcinol may be useful for its keratolytic properties.”
“Emphasis should be placed on barrier-supportive moisturisers containing ceramides. Shaving should be avoided in sensitive areas and patients should avoid harsh scrubs, physical exfoliants, and heavily fragranced products, which may worsen irritation.”
Clothing also plays an important role in managing HS. HidraWear is a company created specifically for sufferers of the condition. The garments specific wound dressing system, makes changing dressings simple for those with flares in the armpit, buttocks and groin.
“For those without access to specialised garments, loose, breathable clothing and non-wired bras can help reduce friction,” says Tan. Ensuring that wound care is managed carefully is essential, and patients should seek advice from a clinician whenever they are uncertain.
Importantly, lifestyle factors should not be underestimated… “Smoking cessation, weight management, balanced diet, and stress management make a real difference,” adds Dr Fabusiwa.
The mental toll of hidradenitis suppurativa
Hidradenitis Suppurativa can have a profound impact on a person’s mental and emotional wellbeing.
“Because HS is chronic, painful, and often unpredictable, many patients live with ongoing fear of flares, embarrassment about drainage or odour, and frustration from delayed diagnoses or ineffective treatments,” says Tan. “The physical discomfort is often accompanied by feelings of shame, isolation, and reduced confidence, especially when lesions occur in intimate or visible areas.”
Being so difficult to manage, HS can interfere with daily activities, relationships, clothing choices, exercise, and work, gradually eroding quality of life.
“Many individuals experience heightened levels of stress, anxiety, and low mood, and some develop depression as a result of long-term pain and social withdrawal. Stigma and misunderstanding from others can compound this, making patients feel unseen or misunderstood.”
“Overall, HS doesn’t just affect the skin, it affects identity, self-esteem, social connection, and emotional resilience. Acknowledging this psychological burden is essential, and compassionate support, mental health resources, and open conversations can make a significant difference in how patients cope and feel supported.”
For those suffering from HS and its symptoms, many guidelines advocate for pain management support and talking therapies.
The future for HS patients
When we were searching for images of HS in Black skin on the widely used stock imagery site Shutterstock, we found nothing apart from the AI image used, but even this portrays an ethnically ambiguous model. This illustrates the extreme need to make dermatology more inclusive.
“Dermatology needs more inclusive research, education, and visibility around hidradenitis suppurativa, especially for women of colour who are disproportionately affected yet underserved,” says Tan.
“I want to see HS represented in medical education the way acne is everywhere, on every skin tone,” adds Dr Fabusiwa. “We need image libraries that show how it really looks on Black skin, more inclusive clinical trials, and honest conversations that remove the stigma.”
“The more we normalise body skin health, the more people will seek help early and that’s where change really begins.”
“Moving forward, medical training should require robust education on diagnosing HS in darker skin, addressing implicit bias, and managing pigmentation and scarring concerns,” says Tan. “Plus, public awareness campaigns and medical resources must feature women of colour to reduce stigma, encourage earlier diagnosis, and ensure they feel seen in the healthcare system.”
You might also like to read... PCOS in Black women: the overlooked realities in beauty and health